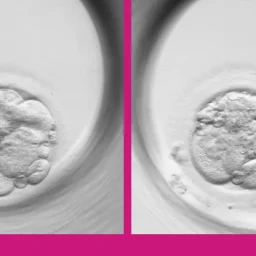
Preimplantation Genetic Diagnosis (PGD) is a procedure used in conjunction with assisted reproduction techniques to screen embryos for chromosome abnormalities. In this way, embryos that are free of genetic disease can be selected prior to transfer. In order to make this diagnosis, a (non-invasive) biopsy must be taken from the embryos to be analysed.
WHEN IS PGD RECOMMENDED?
PGD is recommended in cases where patients have previously had unsuccessful treatments, and where it is suspected that the embryo has an increased risk of chromosome abnormalities. These treatment failures may be related to: repeated miscarriages, advanced maternal age, repeatedly unsuccessful IVF, or males with meiotic abnormalities. It is also indicated for couples carrying sexually transmitted diseases, or with genetic changes in their karyotype (translocations, inversions, etc.), and to prevent the transmission of some monogenic disorders, such as muscular dystrophies, cystic fibrosis or thalassaemia.
The procedure consists of taking one or more cells from the embryo and evaluating them for specific genetic conditions. The results provide information about the chromosome count of the embryos, with the purpose of ruling out monosomies, trisomies, etc. It also enables us to determine if there are structural chromosome abnormalities, or presence of a specific disease that runs in the family.
ADVANTAGES OF PREIMPLANTATION GENETIC DIAGNOSIS
Although originally the biopsy was performed on day 3 of embryonic development (when the embryo is made up of cells called blastomeres), it is currently carried out when the embryo is at the blastocyst stage (the formation of two clearly differentiated structures; the trophectoderm and the inner cell mass).

The reasons for this change in the procedure are as follows:
1. It is important to underline that there will be embryos that have been biopsied on day 3 and are genetically suitable, but cannot be transferred on day 5 because they have not reached the blastocyst stage. However, when embryos are biopsied at the blastocyst stage, they are vitrified and stored in the banks immediately after the biopsy, until the genetic result is obtained. After that, the embryos that are genetically normal can be transferred after devitrification, as they were frozen at a time when they were already suitable for transfer. In this way, patients do not find themselves confronted with the fact that they have embryos which are genetically suitable, but are not at the embryonic development stage for transfer.
2. When the biopsy is performed on day 3, the embryos that are suitable for this technique will ideally have a certain number of cells: eight. Therefore, out of the 8 cells that the embryo has, 1 cell is removed. If the biopsy of the embryo is performed at the blastocyst stage, the number of cells removed will be greater, but with two advantages:
- The number of cells that make up the embryo will be much greater, therefore, even if more cells are removed, they will represent a smaller proportion of the whole cellular constitution of the embryo.
- The biopsy is performed on the area of the trophectoderm, which forms complementary structures in pregnancy, such as the placenta, ensuring that the cells removed are not from the embryonic portion of the blastocyst (inner cell mass).
3. Furthermore, in the case of embryos that have failed to divide normally at some stage of their development, the later the biopsy, the easier it is to detect mosaic embryos, in the same way that false positives and negatives are more common when a single cell is biopsied. In other words, determining as normal those embryos in which the biopsied cell does not carry the abnormality; or determining as genetically abnormal those embryos in which the cell biopsied carried the abnormality, without realising that we are dealing with a mosaic embryo, and many of the others do not carry the abnormality. By removing more cells in a blastocyst biopsy, the risk of not identifying mosaic embryos is minimised.
The grey cells are those that present a genetic alteration, while the pink cells are completely normal. The embryos where both cell types are present are mosaic embryos, and the ratio in which they are found will determine whether or not they are suitable for transfer.
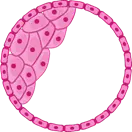
Healthy embryo
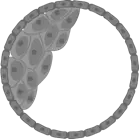
Altered embryo

Mosaic embryo