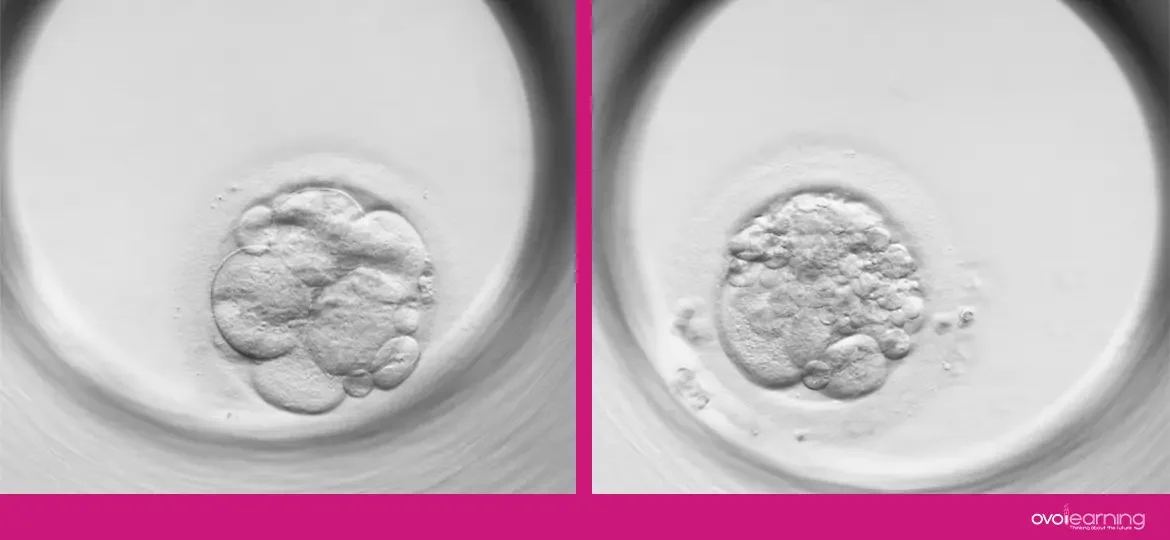
Morphological evaluation by an embryologist is a non-invasive method for transferring embryos, but it involves drawbacks: is highly subjective, requires extensive experience, and is limited to punctual moments of observation within the laboratory routine, implying a loss of information on the overall development of the embryo(1)(2). The main parameters to consider in the morphological evaluation of the embryo before the blastocyst stage are: number and symmetry of cells, degree, and type of fragmentation, and multinucleation(3)(4).
The mechanism of fragmentation remains unknown. It appears that there is a consequence due to a cellular programmed death or apoptosis, which can be observed in fragmented and blocked embryos in their development(5). Fragmentation reduces implantation rates, increases abortion rates, and births of children with chromosomal anomalies (6)(7). What is obvious is that the more fragmentation there is, a greater negative effect and decreased embryonic viability(8).
A fragment is a cytoplasmic extracellular structure that is surrounded by a membrane and lacks a nucleus. Some authors (9) defined the fragments as cells with <45μm diameter in embryos on day 2 and <40μm diameter on day 3 of development (D+3).
It is known that fragmentation may or may not be present at all stages of embryonic development, which is common in all human embryos and is not always associated with a low implantation rate; on the other hand, some authors, despite not establishing a score in their study, state that the absence of fragmentation is associated with a high implantation rate, making this factor more relevant than multinucleation or low embryonic division (Luna, M.D., et al 2008). Other authors ignore this morphological parameter in their classification, giving more importance to the morphology of the zygote in D+1(7), or either they establish an embryonic classification in which nuclear morphology prevails over classical methods based on blastomere size and the degree of fragmentation(10), the Nagy group (11) basing the embryonic selection on morphological parameters in D+3 and in morphology in 2PN.
The implications of embryonic fragmentation on implantation potential vary depending on its distribution and size. The presence of large fragments (type IV fragmentation) is detrimental to embryonic development, while localized or small, dispersed fragments do not significantly affect implantation (12). Authors, such as Jerome (13), believe that the degree of fragmentation or percentage that the pre-embryo that will be transferred may present has no effect on the pregnancy rate. It must be contemplated that this study is designed for unique transferences on women with low reserve, concluding that embryonic implantation is better predicted considering the number and symmetry of blastomeres than considering the degree of fragmentation.
In normal development until blastocyst fragmentation has a negative impact because the type of fragmentation will determine the formation of normal blastocysts, specifically type IV fragmentation led to a significant reduction in blastocyst formation compared to other types of fragmentation (type I, II and III) (14). By contrast, the study conducted by Wu from 2011 (15), establishes a negative correlation between the rate of fragmentation and the development of the blastocyst. Age does not have a positive effect on the degree of fragmentation in correctly divided pre-embryos. The 2006 Martin study (16), supported by studies of Giorgetti de 1995 (17), considered that the pregnancy rate decreases with the increase in the percentage of fragments and establishes two theories on fragmentation: 1) the fragments induce the stoppage of cell development and necrosis of the surrounding blastomeres. 2) intercellular fragments can distort the rhythm of the division of blastomeres, leading to an abnormal compaction, cavitation, and formation of the blastocyst. The embryological parameter that has a direct relation with the implantation potential in D+5, is the established fragmentation in D+3, although it is only a hypothesis to demonstrate. Following the same line of study, the Khurram group (18) considers that a high percentage of fragments (>20%) in D+3 is related to low blastulation rates.
There is no consensus regarding the percentage of fragments, although almost all studies agree on a “cut-off point” associated with the best embryonic quality and a higher rate of implantation (<10% of fragments). In the majority of the articles reviewed, an embryonic score is established where cut-off points for embryonic fragmentation are defined, expressing it as the percentage it occupies with respect to the total embryonic volume. Most authors set this cut-off point to < 10% fragments (19)(20)(21)(14)(22)(23)(24)(25)(26). Other authors set them at < 25% (13) or < 20 %(18)(23). The study of Meseguer (22), establishes several categories considering the degree of fragmentation and the size of blastomeres and multinucleation. Other groups such as Paternot 2013 (27) establish an embryonic classification from the computerized classification, since they consider that there is a high variability between embryologists when the classification is performed according to visualized morphological characteristics. Taking into account these considerations, in terms of fragmentation patterns and embryonic implantation, the last revision of the ASEBIR Morphological Assessment Report (28), establishes four embryo quality groups, according to the fragmentation percentage, volume and distribution of fragments ( 10%, >10-25%, >25-35%, > 35%), recommending those embryos with more than 50% fragmentation should not be cryopreserved or transferred, because its rate of implantation is practically zero. This last consideration was already noted by Nagy’s study (23) which stated that to cryopreserve the pre-embryo, it must have < 20% fragments.
The study of embryonic morphokinetics with the new time-lapse technologies is demonstrating that, to evaluate embryonic quality, both morphological parameters and direct observation must be studied. That is, if morphokinetics allows for more detail in the evaluation. Time-lapse morphokinetics studies, such as Kong’s (29), demonstrate that cell fragmentation and cell division rate are parameters that should be studied together as indicators of embryonic quality, conclusions that were also obtained by other authors such as Ahlstrom (30), where morphology studies by direct observation reach the same conclusion.
Fragment removal (embryonic makeup) appears to improve cell division and implantation. The pioneering group in this technique (31) found that embryos with 35% fragmentation and which had been defragmented implanted at similar rates to those of embryos with only 6% initial fragmentation. The work of Keltz (32) also shows beneficial results, since fragmented embryos and later defragmented presented rates of pregnancy, implantation, and births similar to that of embryos without fragments (not defragmented). In addition, the removal of fragments showed positive effects on the in vitro development of embryos until the sixth day of their development, obtaining blastocysts of better quality (15). However, we must be cautious in the application of this technique since the published studies are scarce and most of them are retrospective.
The study of embryonic morphokinetics using time-lapse technology provides greater precision on the behavior of the embryo during division, noting that the rate of division is relevant for implantation (29), issues that could not be evaluated with traditional embryonic morphological evaluation (temporal observation).
In spite of what the morphokinetics study is providing through time-lapse technology, embryonic quality is defined by the joint evaluation of morphological parameters, as was already the case with traditional morphological evaluation, whether it is true that the morphokinetics study, as already mentioned, provides more detail in the morphological evaluation. Early division together with embryonic fragmentation, according to different authors, are fundamental indicators to categorize the quality of the embryo (29).
And it can be further stated that all studies agree that fragmentation is an important morphological parameter to establish the embryo classification and mostly evaluated in D+2 and D+3. Almost all studies still coincide in a “cut-off point” associated with the best embryonic quality and a higher rate of implantation being <10% of fragments (28). When fragmentation is less than or equal to 10% of the total cell volume (having a better prognosis localized fragmentation versus scattered fragmentation throughout the whole embryonic volume) it does not influence the implantation potential of the pre-embryo.
REFERENCES CONSULTED
- Delgado Mendive M.A. (2015). Relationship between morphological parameters, from gamete to blastocyst, with chromosomal anomalies and reproductive success (Doctoral Thesis). Complutense University of Madrid. Veterinary Faculty. Department of Animal Medicine and Surgery. Recovered from: https://dialnet.unirioja.es/servlet/tesis?codigo=126241
- Delgado A., De Los Santos M., Buendia P., Simon C., Remohi J, & Pellicer A.(2007).Increased incidence of mosaic embryos with the microinjection of spermatozoa with abnormal morphology. Fertil Steril; 88:S229-S230.
- Jurisicova A., Varmuza S., & Casper RF.(1996). Programmed cell death and human embryo fragmentation. Mol Hum Reprod; 2(2):93-8.
- Ebner T., Yaman C., Moser M., Sommergruber M., Pölz W., & Tews G.(2001). Embryo fragmentation in vitro and its impact on treatment and pregnancy outcome. Fertil Steril;76(2):281-5.
- Hardarson, T., Hanson, C., Sjögren, a, & Lundin, K. (2001). Human embryos with unevenly sized blastomeres have lower pregnancy and implantation rates: indications for aneuploidy and multinucleation. Hum Reprod (Oxford, England), 16(2), 313–8. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/11157826.
- Eftekhari-Yazdi P., Valojerdi MR., Ashtiani SK., Eslaminejad MB., & Karimian L. Effect of fragment removal on blastocyst formation and quality of human embryos. Reprod Biomed Online;13(6):823-32.
- Johansson M., Hardarson T., & Lundin K.(2003).There is a cutoff limit in diameter between a blastomere and a small anucleate fragment. J Assist Reprod Genet;20(8):309-313.
- Luna, M., Copperman, A. B., Duke, M., Ezcurra, D., Sandler, B., & Barritt, J. (2008). Human blastocyst morphological quality is significantly improved in embryos classified as fast on day 3 (>or=10 cells), bringing into question current embryological dogma. Fertil Steril, 89(2), 358–63.
- Chen, C., & Kattera, S. (2006). Comparison of pronuclear zygote morphology and early cleavage status of zygotes as additional criteria in the selection of day 3 embryos: a randomized study. Fertil Steril, 85(2), 347–52.
- Haydar N.Ç., Levent K.,Ulun U., Mustafa B., & Faruk B. (2006). Early cleavage morphology affects the quality and implantation potential of day 3 embryos. Fertility and Sterility, 85(2), 358-365.
- Nagy, Z. P., Dozortsev, D., Diamond, M., Rienzi, L., Ubaldi, F., Abdelmassih, R., & Greco, E. (2003). Pronuclear morphology evaluation with subsequent evaluation of embryo morphology significantly increases implantation rates. Fertil Steril, 80(1), 67–74.
- Alikani, M., M., Cohen, J., Tomkin, G., Garrisi, JG., Mack, C., & Scott, R.(1999). Human embryo fragmentation in vitro and its implications for pregnancy and implantation. Fertil Steril, 71(5), 836–42.
- Jerome H. C., Donna S-C., Wei Y., Danya H., & Carrie W.(2007). Effect of embryo quality on pregnancy outcome following single embryo transfer in women with a diminished egg reserve. Fertility and Sterilit;y 87 (4):749-56.
- Alikani M, Calderón G, Tomkin G, Garrisi J, Kokot M, Cohen J. (2000).Cleavage anomalies in early human embryos and survival after prolonged culture in-vitro. Hum Reprod 2000;15:2634-2643.
- Wu, D. H., Reynolds, K., Maxwell, R., Lindheim, S. R., Aubuchon, M., & Thomas, M. a. (2011). Age does not influence the effect of embryo fragmentation on successful blastocyst development. Fertil Steril, 95(8), 2778–80.
- Martin D. K., Josh C. S.,Katrina B., Daniel S.(2006). Predictors of embryo fragmentation and outcome after fragment removal in in vitro fertilization. Fertil Steril, 86(2), 321–24.
- Giorgetti C., Terriou P., Auquier P., Hans E., Spach J.L., Salzmann J., & Roulier R.(1995). Embryo score to predict implantation after in-vitro fertilization: based on 957 single embryo transfers. Hum Reprod;10(9):2427-31.
- Khurram S. R., Orhan B., Martin L., Bruce R. C., Anna C. N., Kathleen M. D., Kevin J. D.(2007). Late stages of embryo progression are a much better predictor of clinical pregnancy than early cleavage in intracytoplasmic sperm injection and in vitro fertilization cycles with blastocyst-stage transfer. Fertility and Sterility; 87 (5): 1041-52.
- Della Ragione, T., Verheyen, G., Papanikolaou, E. G., Van Landuyt, L., Devroey, P., & Van Steirteghem, A. (2007). Developmental stage on day-5 and fragmentation rate on day-3 can influence the implantation potential of top-quality blastocysts in IVF cycles with single embryo transfer. Reproductive biology and endocrinology: RB&E, 5, 2.
- Hnida, C. (2004). Computer-controlled, multilevel, morphometric analysis of blastomere size as biomarker of fragmentation and multinuclearity in human embryos. Hum Reprod, 19(2), 288–293.
- Holte, J., Berglund, L., Milton, K., Garello, C., Gennarelli, G., Revelli, a, & Bergh, T. (2007). Construction of an evidence-based integrated morphology cleavage embryo score for implantation potential of embryos scored and transferred on day 2 after oocyte retrieval. Hum Reprod (Oxford, England), 22(2), 548–57.
- Meseguer, M., Herrero, J., Tejera, A., Hilligsøe, K. M., Ramsing, N. B., & Remohí, J. (2011). The use of morphokinetics as a predictor of embryo implantation. Hum Reprod (Oxford, England), 26(10), 2658–71.
- Nagy, Z. P., Taylor, T., Elliott, T., Massey, J. B., Kort, H. I., & Shapiro, D. B. (2005). Removal of lysed blastomeres from frozen-thawed embryos improves implantation and pregnancy rates in frozen embryo transfer cycles. Fertil Steril, 84(6), 1606–12.
- Pelinck, M.-J., Hoek, A., Simons, A. H. M., Heineman, M. J., van Echten-Arends, J., & Arts, E. G. J. M. (2010). Embryo quality and impact of specific embryo characteristics on ongoing implantation in unselected embryos derived from modified natural cycle in vitro fertilization. Fertil Steril, 94(2), 527–34.
- Van Royen, E., Mangelschots, K., De Neubourg, D., Laureys, I., Ryckaert, G., & Gerris, J. (2001). Calculating the implantation potential of day 3 embryos in women younger than 38 years of age: a new model. Hum Reprod (Oxford, England), 16(2), 326–32. Retrieved from: https://pubmed.ncbi.nlm.nih.gov/11157828/
- Ziebe, S., Petersen, K., Lindenberg, S., Andersen, a G., Gabrielsen, a, & Andersen, a N. (1997). Embryo morphology or cleavage stage: how to select the best embryos for transfer after in-vitro fertilization. Hum Reprod (Oxford, England), 12(7), 1545–9. Retrieved from: https://pubmed.ncbi.nlm.nih.gov/9262293/
- Paternot, G., Debrock, S., De Neubourg, D., D`Hooghe, T.M, Spiessens,C. (2013). Semi-automated morphometric analysis of human embryos can reveal correlations between total embryo volume and clinical pregnancy. Hum Reprod (Oxford, England); 28(3): 627–33.
- ASEBIR. (2015). Criterios ASEBIR de Valoración Morfológica de Oocitos, Embriones Tempranos y Blastocistos Humanos 3ª Edición. Madrid. Góbalo.
- Kong X., Yang S., Gong F., Lu C., Zhang S., Lu G., Lin G. (2016). The Relationship between Cell Number, Division Behavior and Developmental Potential of Cleavage Stage Human Embryos: A Time-Lapse Study. PLoS One.14;11(4): e0153697. doi: 10.1371/ journal.pone.0153697. eCollection 2016.
- Aisling A., Hannah P., Christina B., Ulrika S., Kersti L.(2016). Conventional morphology performs better than morphokinetics for prediction of live birth after day 2 transfer. Reprod Biomed Online. 2016 Jul;33(1):61-70. doi: 10.1016/j.rbmo.2016.03.008. Epub 2016 Apr 7.













